As the world still holds its breath for the widespread rollout of COVID-19 vaccines, the experts studying infectious diseases are already shifting their focus to the prevention of the next pandemic.
While this may seem pessimistic to those eager to celebrate the expected suppression of COVID-19 and a hopeful return to pre-pandemic life, researchers in the realms of biology and epidemiology have adopted a more realistic approach. Irrespective of their specific field of focus, a persistent question circulates among the experts: not if there will be another pandemic, but when.
As Bill Gates noted in recent commentary, “We don’t know when the next one will strike, or whether it will be a flu, a coronavirus, or some new disease we’ve never seen before. But what we do know is that we can’t afford to be caught flat-footed again. The threat of the next pandemic will always be hanging over our heads—unless the world takes steps to prevent it.”
The first step we must take involves close examination of the factors which increase risk.
While human interconnectedness in an increasingly globalized world certainly enables the spread of infectious diseases, the most prominent (and as yet, unaddressed) threats to human health arise from proximity to viruses infecting livestock and other animals. In fact, 75% of emerging diseases are zoonotic—and the ever-present risk that one of these strains may evolve into the next global pandemic increases as climate change, habitat encroachment, overpopulation and urbanization continue to alter our interaction with the natural world.
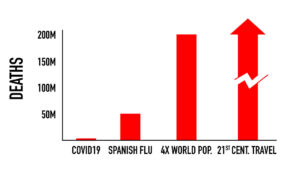
SARS-CoV-2 (the virus that causes COVID-19) has an average mortality rate that is actually quite low when compared to the potential impact of other known viral threats. For instance, Middle East Respiratory Syndrome (MERS), a virus that initially spread to humans from infected camels kept as livestock, has an average mortality rate of 35%. And the Nipah virus (which has seen documented transmission to humans from both pigs and bats) carries a mortality rate as high as 75%.
Thus far, we’ve been fortunate that these species-jumping bugs have been constrained by lower rates of transmission. To quote a recent interview with Christian Walzer, Executive Director of Health at the Wildlife Conservation Society, on the subject of MERS, “What keeps me up at night is the possibility that another coronavirus—like MERS, which has a much, much higher mortality rate—becomes as transmissible as COVID. The logistics and the psychological trauma of that would be unbearable.”
In order to protect the lives of humans worldwide, it is imperative that we shift from historically reactive responses to viral threats, to a mindset of proactive preparation. The introduction of effective prophylactic measures, such as mandatory influenza testing and vaccination of farmed animals, is an excellent start. So is increasing the attention and funding devoted to efforts that identify zoonotic threats, such as the Global Virome Project. Support of initiatives that track the spread, containment and impact of animal illnesses is also essential.
The threat posed by new outbreaks is continuous. Whether by viruses or pathogens new or undiscovered, COVID-19 has demonstrated how quickly pandemic-level exposure can be achieved, once the human barrier has been breached.
According to experts at the University of Kent, “If we want to prevent future pandemics that are similar to or even worse than COVID-19, we will need strategies that go far beyond previous preparedness plans and that enable us to take strong actions immediately.”
Consideration of the patterns and means of human-to-human transmission is critical to the evolution of strong containment strategies. Effective methodologies and tools for contact tracing must undergo proactive development and adoption if we wish to empower communities to contain pandemic spread.
Increased financial support for research focused on viral sequencing and vaccine development must be prioritized by global health initiatives and government entities. Streamlined approval for life-saving vaccines and drugs, as well as nimble, strategic coordination of widespread distribution, is imperative.
A strong, cohesive response to the next global pandemic hinges on increased international financing, governmental cooperation, and scientific collaboration. As COVID-19 has proven, only a strategic, informed and globally coordinated response will empower us to mitigate future epidemiological threats.
With careful consideration, our current encounter with COVID-19 can be mined for lessons that define, strengthen and inform our future approach. Though there are myriad factors in this complex equation, with careful accounting the resulting formula will help us limit the impact and damage caused by the next pandemic—and save countless lives.